Share:
What is an Age-Friendly Health System?
 As you may know by now, Asante Ashland Community Hospital is in the process of achieving an Age-Friendly Health System designation. While most of us know what it means to become a pediatric, orthopedic or long-term care hospital, being age-friendly is perhaps less familiar.
As you may know by now, Asante Ashland Community Hospital is in the process of achieving an Age-Friendly Health System designation. While most of us know what it means to become a pediatric, orthopedic or long-term care hospital, being age-friendly is perhaps less familiar.
While the precise details of what this will mean for AACH will be evolving over the coming months and years, a good place to start is to understand what exactly an Age-Friendly Health System is. It’s an international initiative funded by the John A. Hartford Foundation and the Institute for Healthcare Improvement with the American Hospital Association and the Catholic Health Association of the United States.
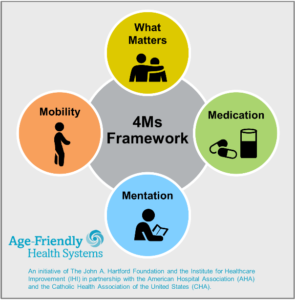
The designation provides health care systems with the framework to transform care that is delivered to older adults. It is a model built on the “Four Ms”: What matters most, medication, mentation and mobility. It shifts the focus from being centered on the disease to being centered on the person.
What matters most to the patient
In an Age-Friendly Health System, this is where all care starts. It is key to know and to act on each older adult’s specific health outcome goals and care preferences. Providers and staff make sure to understand a different set of questions in addition to health history and medications. These questions may be “What is important to you aside from health care?” Or, “What brings you joy? Makes you happy? Makes life worth living?” These questions may seem simplistic, or even a waste of valuable time. However, in an age-friendly setting, the answers drive everything that follows.
Medications
On admission to an Age-Friendly hospital, patients are generally assessed for high-risk medications. This assessment continues anytime new medications are added and include the bedside nurse staff and pharmacist, as well as the physician. High risk medications, those that are likely to cause delirium in older adults, are avoided or minimized. Pharmacists and physicians partner together to find age-friendly medications that do not interfere with what matters, mobility or mentation. When possible, an Age-Friendly hospital will even work to deprescribe medications when appropriate.
Mobility
This is key for our older adults in an age-friendly setting. Nursing staff and physical therapy often partner together to set mobility goals, avoid high-risk medications that might result in a patient being “too drugged” for physical therapy and other measures. Some Age-Friendly hospitals even have small group exercise classes for patients.
Mentation
In the hospital setting, this means preventing delirium. Age-Friendly hospitals prioritize assessing patients for delirium and take all steps necessary to avoid is. The keys to this are simple and generally revolve around:
- Identifying and treating underlying causes
- Assuring safety
- Gently re-orienting the patient
- Ensuring hydration
- Promoting sleep
- Increasing ambulation
Chemical and physical restraints are avoided. Some Age-Friendly hospitals also work to encourage socialization among patients to prevent isolation and confusion.
Again, while we haven’t decided exactly how the Age-Friendly Health System designation will look like at AACH, hopefully this article gives you a sense of what we are hoping to achieve. This will be a process that will require us to assess where we are today and then plan for where we want to be tomorrow.
If you have a question, please contact the author or relevant department directly.




1 Comment. Leave new
I love the concept!!