Share:
Asante has taken on an ambitious effort to ease the opioid crisis
“The best time to repair the roof is when the sun is shining.” — John F. Kennedy in the 1962 State of the Union Address, a year after the recession.
When the U.S. economy gleamed in 2019, a year preceding the dual crises of the viral pandemic and opioid epidemic, our national job growth was soaring toward its 10th annual peak since the financial crisis.
During that year in bloom, questions murmured in Asante Pharmacy and small-group discussions about our approach to caring for a pool of high-risk patients: How well are we managing their acute pain with opioids, especially among postoperative patients? And perhaps more pressingly, what can we do to encourage safe, effective opioid use in our system and our communities?
These inquiries spawned the development of our opioid stewardship initiative, a multi-team effort conceived by Amy Watson, Asante director of Pharmacy Services and chief pharmacy officer.
“Medications that are critical to appropriate care but dangerous when not used appropriately require thoughtful stewardship,” Watson cautions. “Opioids were a natural place to focus.”
Watson envisioned the need to prioritize and scope Asante’s collaborative work on opioid stewardship. “We needed to focus carefully on the areas we could impact to help our communities. We needed a diverse team of people to make a difference.”
Although billions of federal dollars and immeasurable dreams have been invested in tandem with the CMS’s national strategy to address the opioid crisis, the meteoric rates of opioid-related admissions and mortality have curiously remained unrelenting in intensity and magnitude.
A recent national study reported that most patients with opioid use disorders, or OUD, did not receive proper hospital-based opioid treatment on admission or discharge. This would have baffled health care teams if these patients were to present hypothetically in an alternative scenario with stroke or sepsis.
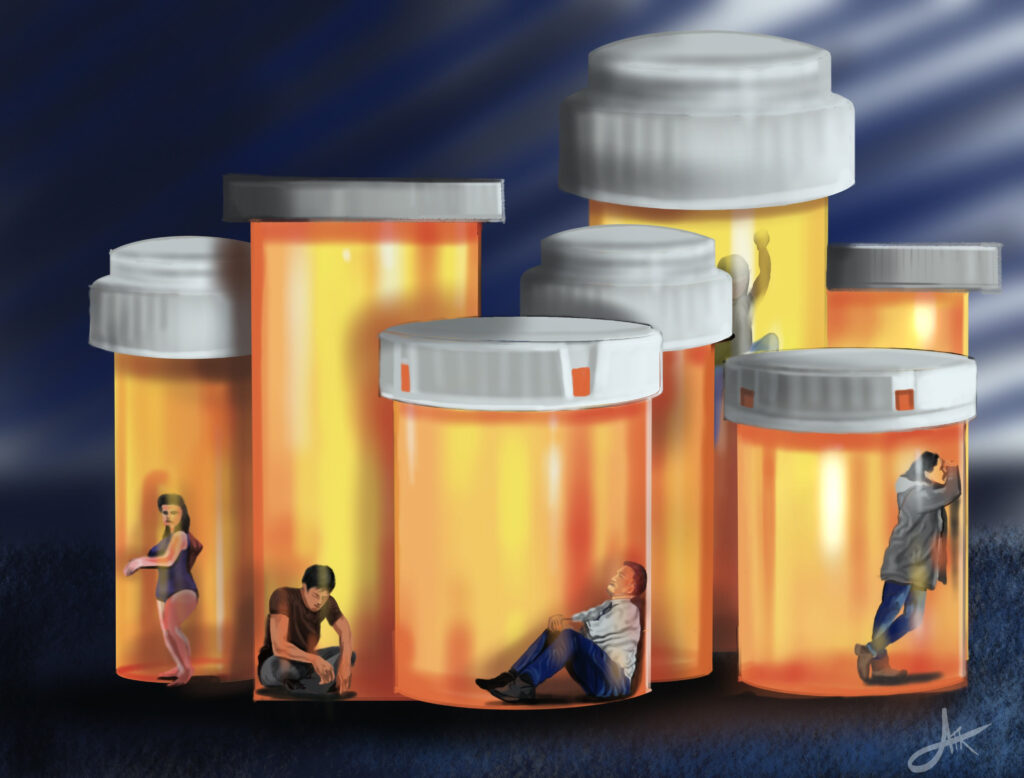
To help demystify the complexities of OUD patients that transcend a diagnosis, ARRMC hospitalist Arun Kuruvila, MD, whose art has been showcased in the Annals of Internal Medicine and locally at Roxy Ann Winery and South Stage Cellars, digitally paints the haunting narratives of OUD patients to rekindle honest, hard conversations.
A gifted painter since childhood, Dr. Kuruvila illustrates the opioid crisis through creative art, shattering shame with his contours of ordinary people in despair. His work can be seen on the Addiction Opioid hub![]() on myAsanteNET and in the images above.
on myAsanteNET and in the images above.
“I have seen the damage done by opioids to many of my patients,” he shares. “About 75% of all overdose deaths are from opioids and the number is rapidly increasing.”
At a recent town hall meeting with the City of Medford, Erin Brender, MD, an ARRMC hospitalist and Epic physician liaison, rallied the need for hospital-based opioid therapy.
“Admission is a reachable moment at the point of care when patients are more likely to want to engage in a highly effective treatment,” says Dr. Bender, who has been championing Asante’s Learning Collaborative on OUD with Oregon Health & Science University. “Most patients with high-risk drug use want to cut back or quit. Having this program in place helps prevent patients from falling through the cracks.”
Focus yields benefits
Dr. Brender’s leadership in the collaborative with Asante and community partners has begun to reap emerging results.
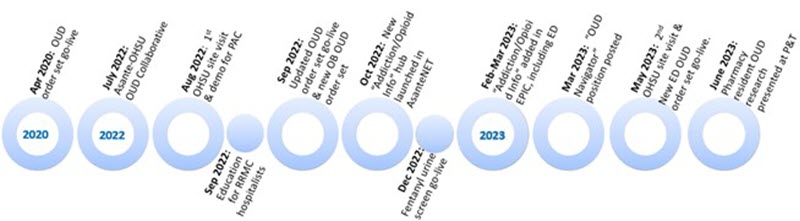
Milestones in hospital-based opioid treatment, or HBOT.
In the Emergency Department over the past several months, Danielle Holtz, MD, designed a new OUD order set with Tim Peterson, Epic senior analyst and pharmacist, and her ED team to help transition patients from the ED to medication-assisted treatment clinics.
“With the increasing prevalence of fentanyl use in the community, this order set streamlines the management of acute opioid withdrawal and helps physicians and nurses in the ED become more comfortable treating these often complex patients,” Holtz details.
Since ED nurses have not been historically acquainted with applying Clinical Opioid Withdrawal Scale (COWS) to gauge opioid withdrawal symptoms, Kyla Peterson, Advanced Practice Registered Nurse (APRN) in ED, has been educating them about monitoring, treatment and documentation:
“ED nurses are getting the education to treat symptoms of withdrawal and help patients feel more comfortable when going through withdrawal. They will now have a better understanding of the COWS assessment and will have quick access to this COWS assessment in the ED Narrator.”
For pregnant women with OUD, Kerri Hecox, MD, medical director of Oasis Center of the Rogue Valley, has partnered with ARRMC’s Family Birth Center to create an innovative program melding principle and practice.
“The Family Birth Center has made tremendous progress in optimizing care for these patients,” Dr. Hecox explains. “On July 1, the Oasis Center will open a six-bed emergency housing unit for pregnant women with substance use disorders in need of safe housing as they transition into recovery.”
As Asante celebrates each milestone in step with the CMS roadmap grounded on the “harm reduction” model, our momentum to dismantle guilt, regret and stigma — three key barriers to recovery — is helping to change perspectives and renew lives.
“By offering patients medication-assisted treatment, we are treating opioid addiction as the disease that it is,” affirms Steven Hersch, MD, AACH’s vice president of Medical Affairs and physician champion for opioid stewardship. This calls for individual and communal resilience. “Patients can confront their disease directly and begin their healing process while hospitalized.”
If you have a question, please contact the author or relevant department directly.





4 Comments. Leave new
Thank you for this article! I have always wondered how our Asante pharmacy and clinical teams are working to manage the opioid crisis. As an IT worker, I am removed from this crisis professionally but see the devastation it wreaks in individuals, families and society. Dr. Kuvila’s art was an added bonus; it truly reflects the pathos of this situation – the isolation and tall obstacles of addiction. I could not have guessed you are doing so much to address opioid use – which starts as a physical pain reliever, but ultimately can cause so many other types of pain. Thank you for your work and taking the time to let us all know how Asante is trying to help.
Wow! Dr. Kuruvila’s artwork is so evocative.
Well written article on how Asante is doing its part in addressing the epidemic of opioid abuse. Assisting patients that become addicted to prescribed opioids is one thing, responding to the tidal wave of opioid experimentation by youth is another. Since this problem is common across the country, federal funding should be available to support these efforts of Asante. Federal funding aside, Asante is to be commended for tackling such a disastrous healthcare crisis.
This is a wonderful article, it just strikes me as odd that there’s no mention that there have been three nurse practitioners at family medicine on Murphy Road, who have single-handedly been trying to combat the opioid crisis for the past six years, by becoming data waivered-(which is no longer necessary, and any primary care physician can prescribe medication to treat opioid use disorder). We have been fighting to get Sublocade, an injectable medication, used to treat opioid use disorder, which is still not approved by Asante. I am happy to see that people are taking this crisis more seriously, and I sure hope to see more primary care providers, offering to treat medication use disorder with Suboxone.