Share:
How we’re solving our capacity challenges
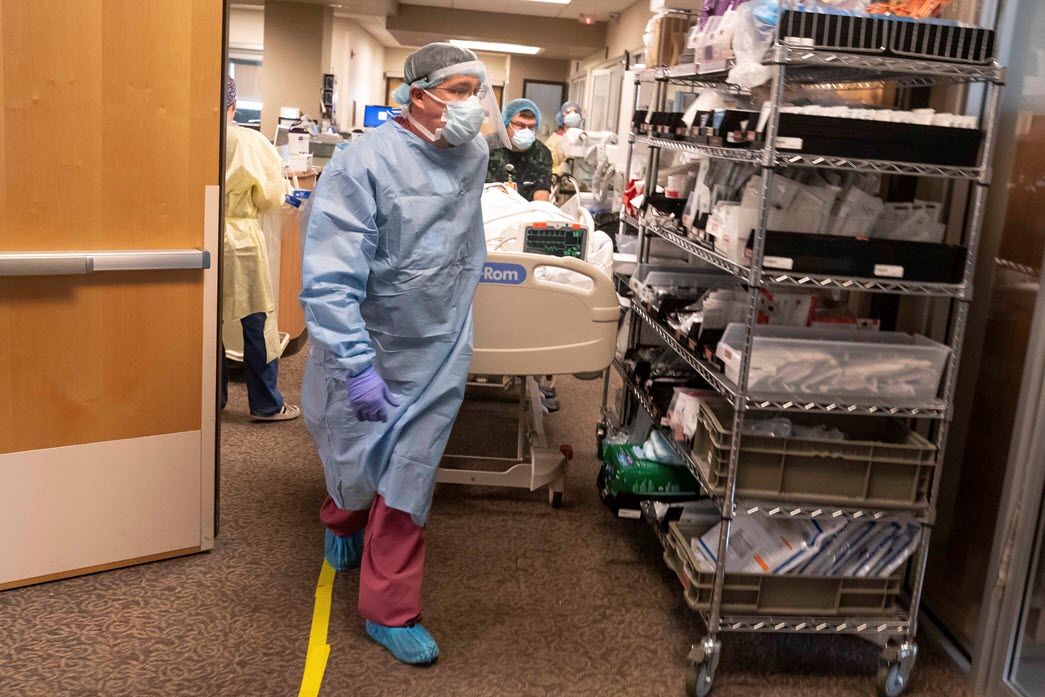
There is no doubt that our COVID-19 hospitalizations are much lower than during the peak delta and omicron surges, yet Asante’s hospitals are still struggling with high volumes of patients, which is having a major impact on our health system.
Even with the daily capacity challenges we face, our goal remains the same: Ensure our patients receive care without delay.
The capacity situation
Systemwide, we are over 100% hospital occupancy on a regular basis. In fact, we haven’t been below 80% capacity since 2020.
Capacity issues are felt in several ways, including more boarders in our emergency departments; delayed or canceled surgeries and procedures; a decreased ability to accept regional referrals; and a buildup of inpatients awaiting discharge to a long-term care or skilled nursing facility.
High patient volumes also result in our use of temporary surge beds to safely care for patients, as well as heighten the potential for negative impacts to our quality and patient experience initiatives.
The impact of high-capacity
The demand for beds is greater than the number of beds available. The pandemic has shown us there are not enough long-term care and skilled nursing facility beds in Southern Oregon. As a result, most weeks we have between 35 and 40 patients awaiting placement who no longer require hospital-level care.
Our hospital bed volume also affects our ability to move patients out of the emergency department and surgical/procedural areas in a timely manner. ARRMC had record-high days in June, with 42 boarders in our Emergency Department waiting for an inpatient bed.
Our hospitals have seen a slight rebound in emergency department use and procedural and surgical growth since COVID caused those volumes to drop. We’ve also seen an improvement in our ability to accept transfers since March, despite our high volumes.
Our actions and solutions
Even with these challenges, our teams are working tirelessly to manage our patient volume. Their strong capacity management and coordination of our system resources will determine how effectively we serve our community in the future.
A few examples of the work being done include:
- Load balancing. Minimize the time when one entity is nearing critical capacity while another facility has a high availability of beds. Evaluate short-, medium- and long-term capacity strategies to accommodate surges across our hospitals.
- Discharge planning. Document the estimated date of discharge that the whole care team works toward. Predicting a discharge date allows us to shorten the patient’s length of stay and free up a bed sooner, possibly for a surgery patient or boarder in the emergency department.
- Emergency licensure. A special-purpose renal dialysis facility certificate has been granted to Asante. This allows us to temporarily provide outpatient dialysis to patients who cannot get discharged to community-based dialysis due to a lack of available services.
- Skilled nursing facility. A contract with community-based Prestige ensures us the use of 20 beds to place our patients who need to be discharged to a step-down level of care.
These are just a few of the measures we’ve taken to address the high volume of patients in our hospitals; there are many more. Another factor that affects capacity is staffing. We are aggressively recruiting clinic staff in all areas in order to reduce traveler hours.
Please be assured that Asante’s leaders at all levels continue to seek and find solutions to meet the demand for care and ensure our patients get the care they need — when they need it.
If you have ideas to share, I encourage you to talk with your supervisor. Your input will make a difference.
If you have a question, please contact the author or relevant department directly.



